Vitamin D deficiency may actually contribute to Crohn's disease because the hormone modulates the immune system. According to endocrinologists at McGill University, vitamin D appears to turn on genes to encode antimicrobial peptides that fight against intestinal invaders (1). The immune support may help avoid inflammation associated with an autoimmune response in Cronh's disease.
This may explain why Crohn's disease is more prevalent in Northern latitude countries. It also suggests that increased vitamin D could assist in avoiding Crohn's disease in the future.
How do these findings affect what we know about ulcerative colitis? I hope we find out soon.
Reference
1. McGill University Health Centre (2010, January 27). Vitamin D supplements could fight Crohn's disease. ScienceDaily. Retrieved March 31, 2010, from http://www.sciencedaily.com /releases/2010/01/100127104904.htm
Wednesday, March 31, 2010
Managing Diverticulitis After Treatment
It is well documented that a diet low in insoluble fiber is considered the main etiological factor in leading to diverticulitis. The intake of insoluble fiber speeds up transit of food and increases bulk reducing pressure on the intestine (1). On the other hand, intake of red meat appears to increase risk (1).
Patients treated for diverticulits are often prescribed antibiotic therapy and recommended to stay on a low-fiber diet and reintroducing insoluble fiber gradually (2). In some cases, surgery is needed (2). Afterward, nutritionists would recommend gradual increases of fiber because a diet high in fiber can lead to high amounts of gas and forceful diarrhea (2-3).
Because of possible damage in the intestine, nutritionists should also evaluate patients are at higher risk of malnutrition. Malnutrition can lead to slow healing and recovery as well as deterioration of muscle, respiratory and immune function (4). To receive adequate nutrients, higher protein intake as well as supplements of certain vitamins such as B12 and minerals such as calcium may be needed (4).
A weight-management program may help to avoid diverticulitis in the future. According to a prospective cohort study, subjects with a BMI, waist circumference and waist-to-hip ratio that categorized them as obese had an increased risk of diverticulitis and diverticular bleeding (5).
Nutritionists may also recommend probiotics along with prebiotics to support growth of healthy intestinal flora after antibiotic therapy (4).
References
1. Korzenik JR. Case closed? Diverticulits: epedemiology and fiber. J Clin Gastroeneterol. 2006 Aug;40 Suppl 3:S1 12-6.
2. Kotzampassakis N, Pittet O, Schmidt S, Denys A, Demarines N, Calmes JM. Presentation and treatment outcome of diverticulitis in younger adults: a different disease than in older patients? Dis Colon Rectum. 2010 Mar;53(3):333-8.
4. Kohlstadt I. Food and Nutrients in Disease Management. Boca Raton, FL: CRC Press, 2009.
5. Strate LL, Liu YL, Aldoori WH, Syngal S, Giovannucci EL. Obesity increases the risks of diverticulitis and diverticular bleeding 2008;136(1):115-112.
Patients treated for diverticulits are often prescribed antibiotic therapy and recommended to stay on a low-fiber diet and reintroducing insoluble fiber gradually (2). In some cases, surgery is needed (2). Afterward, nutritionists would recommend gradual increases of fiber because a diet high in fiber can lead to high amounts of gas and forceful diarrhea (2-3).
Because of possible damage in the intestine, nutritionists should also evaluate patients are at higher risk of malnutrition. Malnutrition can lead to slow healing and recovery as well as deterioration of muscle, respiratory and immune function (4). To receive adequate nutrients, higher protein intake as well as supplements of certain vitamins such as B12 and minerals such as calcium may be needed (4).
A weight-management program may help to avoid diverticulitis in the future. According to a prospective cohort study, subjects with a BMI, waist circumference and waist-to-hip ratio that categorized them as obese had an increased risk of diverticulitis and diverticular bleeding (5).
Nutritionists may also recommend probiotics along with prebiotics to support growth of healthy intestinal flora after antibiotic therapy (4).
References
1. Korzenik JR. Case closed? Diverticulits: epedemiology and fiber. J Clin Gastroeneterol. 2006 Aug;40 Suppl 3:S1 12-6.
2. Kotzampassakis N, Pittet O, Schmidt S, Denys A, Demarines N, Calmes JM. Presentation and treatment outcome of diverticulitis in younger adults: a different disease than in older patients? Dis Colon Rectum. 2010 Mar;53(3):333-8.
4. Kohlstadt I. Food and Nutrients in Disease Management. Boca Raton, FL: CRC Press, 2009.
5. Strate LL, Liu YL, Aldoori WH, Syngal S, Giovannucci EL. Obesity increases the risks of diverticulitis and diverticular bleeding 2008;136(1):115-112.
Helping a Patient Manage IBS and Diarrhea
When IBS is diarrhea-predominant, a doctor may prescribe an antimotility agent to assist patients with symptoms (1). He or she may also prescribe an antibiotic if the IBS is a result of small intestinal bacterial overgrowth (1).
As a dietary aid for patients, a nutritionist may suggest soluble fiber such as from oats because it can help act against symptoms such as diarrhea by helping bind fat and slow emptying of food from the stomach into the small intestine (2).
The soluble fiber can include prebiotics such as fructo-oligosaccharides or resistant maltodextrin, which support growth of healthy intestinal bacteria. The prebiotics taken in conjunction with probiotics particularly after antibiotic therpay may help with promoting the growth of the good bacteria. This integrative therapy can help to alleviate symptoms by promoting competition against small intestinal bacterial growth (3).
Nutrionists should recommend suspending intake of insoluble fiber such as from wheat and cereal grains and limiting poorly-digested carbohydrates and sugar alcohols as these can worsen symptoms (4). Patients may find benefit from following an exclusion diet whereas trigger foods are eliminated and then, if thought advisable, reintroduced gradually (4).
References
1. Kohlstadt I. Food and Nutrients in Disease Management. Boca Raton, FL: CRC Press, 2009.
2. Bijkerk CJ, de Wit NJ, Muris JWM, Whorwell PJ, Knottnerus JA, Hoes AW. Soluble or insoluble fibre in irratble bowel syndrome in primary care? Randomized placebo controlled trial. Brit Med Jour 2009;339:b3154. Available at http://www.bmj.com/cgi/content/abstract/339/aug27_2/b3154. Accessed on March 31, 2010.
3. American College of Gastroenterology (2008, October 10). How Effective Are Probiotics In Irritable Bowel Syndrome?. ScienceDaily. Available at http://www.sciencedaily.com /releases/2008/10/081006092656.htm. Accessed on March 31, 2010.
4. Heizer WD, Southern S, McGovern S. The role of diet in symptoms of irritable bowel syndrome in adults: a narrative view. J Am Diet Assoc. 2009 Jul;109(7):1204-1.
As a dietary aid for patients, a nutritionist may suggest soluble fiber such as from oats because it can help act against symptoms such as diarrhea by helping bind fat and slow emptying of food from the stomach into the small intestine (2).
The soluble fiber can include prebiotics such as fructo-oligosaccharides or resistant maltodextrin, which support growth of healthy intestinal bacteria. The prebiotics taken in conjunction with probiotics particularly after antibiotic therpay may help with promoting the growth of the good bacteria. This integrative therapy can help to alleviate symptoms by promoting competition against small intestinal bacterial growth (3).
Nutrionists should recommend suspending intake of insoluble fiber such as from wheat and cereal grains and limiting poorly-digested carbohydrates and sugar alcohols as these can worsen symptoms (4). Patients may find benefit from following an exclusion diet whereas trigger foods are eliminated and then, if thought advisable, reintroduced gradually (4).
References
1. Kohlstadt I. Food and Nutrients in Disease Management. Boca Raton, FL: CRC Press, 2009.
2. Bijkerk CJ, de Wit NJ, Muris JWM, Whorwell PJ, Knottnerus JA, Hoes AW. Soluble or insoluble fibre in irratble bowel syndrome in primary care? Randomized placebo controlled trial. Brit Med Jour 2009;339:b3154. Available at http://www.bmj.com/cgi/content/abstract/339/aug27_2/b3154. Accessed on March 31, 2010.
3. American College of Gastroenterology (2008, October 10). How Effective Are Probiotics In Irritable Bowel Syndrome?. ScienceDaily. Available at http://www.sciencedaily.com /releases/2008/10/081006092656.htm. Accessed on March 31, 2010.
4. Heizer WD, Southern S, McGovern S. The role of diet in symptoms of irritable bowel syndrome in adults: a narrative view. J Am Diet Assoc. 2009 Jul;109(7):1204-1.
Tuesday, March 30, 2010
Adiponectin supplementation: Body fat loss
Adiponectin is a hormone exclusively secreted by body fat. This hormone has been recently gaining attention from researchers because of some of its functions. Two important ones are the regulation of glucose and fat metabolism.
Elevated levels of adiponectin are associated with increased insulin sensitivity, and increased fat catabolism (i.e., fat burning). And these associations appear to be causal. That is, adiponectin levels do not seem to be only markers, but causes of increased insulin sensitivity and fat catabolism.
In other words, an increase in circulating adiponectin seems to lead to increased insulin sensitivity and increased fat catabolism. Insulin sensitivity is the opposite of insulin resistance. The latter is a precursor to diabetes type 2, and is associated with elevated fasting and postprandial (i.e., after a meal) glucose levels.
Adiponectin also seems to work closely with leptin, another hormone implicated in a number of diseases of civilization. It appears that adiponecting and leptin modulate each other’s secretion and effects in metabolic processes.
So what do we do to increase our levels of circulating adiponectin?
Well, apparently there is only one guaranteed way, and that is to lose body fat!
Adiponectin is unique among hormones secreted by body fat in that it increases as body fat decreases. Other important body fat hormones, such as leptin, decrease with body fat loss.
The figure below (from: Poppitt et al., 2008) shows a graph where adiponectin levels are plotted against body mass index (BMI). BMI is strongly correlated with body fat percentage.
As you can see from the figure above adiponectin levels more than double when BMI goes from 26 to 20. One does not need to be obese to take advantage of this effect, and to benefit from having increased adiponectin levels.
The linear (Pearson) correlation between BMI and adiponectin levels is indicated as a high 0.551. The fluctuations around the line (the "line" looks more like a quasi-linear curve obtained through quadratic regression), which are why the correlation is not 1, are probably due chiefly to two factors:
- BMI is not a very precise measure of body fat. A very muscular person will have a high BMI and low body fat. That person will consequently have much higher adiponectin levels than an obese person with equal BMI.
- Adiponectin levels are naturally higher in women than in men. This is another point in favor of adiponectin, as women have always been the evolutionary bottleneck among our Paleolithic ancestors.
Now you know why doctors prescribe weight loss to patients with diabetes type 2.
And, when we look at various hunter-gatherer groups that were apparently free of diseases of civilization prior to westernization, there are only a few common denominators. Diet was not one of them, as Weston Price and others have shown us, at least not in the sense of what they included in their diet.
One of the few common denominators was arguably the fact that those hunter-gatherers typically had relatively low levels of body fat; an almost universal feature among non-westernized hunter-gatherers.
Reference:
Poppitt, S.D. et al. (2008). Postprandial response of adiponectin, interleukin-6, tumor necrosis factor-α, and C-reactive protein to a high-fat dietary load. Nutrition, 24(4), 322-329.
Elevated levels of adiponectin are associated with increased insulin sensitivity, and increased fat catabolism (i.e., fat burning). And these associations appear to be causal. That is, adiponectin levels do not seem to be only markers, but causes of increased insulin sensitivity and fat catabolism.
In other words, an increase in circulating adiponectin seems to lead to increased insulin sensitivity and increased fat catabolism. Insulin sensitivity is the opposite of insulin resistance. The latter is a precursor to diabetes type 2, and is associated with elevated fasting and postprandial (i.e., after a meal) glucose levels.
Adiponectin also seems to work closely with leptin, another hormone implicated in a number of diseases of civilization. It appears that adiponecting and leptin modulate each other’s secretion and effects in metabolic processes.
So what do we do to increase our levels of circulating adiponectin?
Well, apparently there is only one guaranteed way, and that is to lose body fat!
Adiponectin is unique among hormones secreted by body fat in that it increases as body fat decreases. Other important body fat hormones, such as leptin, decrease with body fat loss.
The figure below (from: Poppitt et al., 2008) shows a graph where adiponectin levels are plotted against body mass index (BMI). BMI is strongly correlated with body fat percentage.
As you can see from the figure above adiponectin levels more than double when BMI goes from 26 to 20. One does not need to be obese to take advantage of this effect, and to benefit from having increased adiponectin levels.
The linear (Pearson) correlation between BMI and adiponectin levels is indicated as a high 0.551. The fluctuations around the line (the "line" looks more like a quasi-linear curve obtained through quadratic regression), which are why the correlation is not 1, are probably due chiefly to two factors:
- BMI is not a very precise measure of body fat. A very muscular person will have a high BMI and low body fat. That person will consequently have much higher adiponectin levels than an obese person with equal BMI.
- Adiponectin levels are naturally higher in women than in men. This is another point in favor of adiponectin, as women have always been the evolutionary bottleneck among our Paleolithic ancestors.
Now you know why doctors prescribe weight loss to patients with diabetes type 2.
And, when we look at various hunter-gatherer groups that were apparently free of diseases of civilization prior to westernization, there are only a few common denominators. Diet was not one of them, as Weston Price and others have shown us, at least not in the sense of what they included in their diet.
One of the few common denominators was arguably the fact that those hunter-gatherers typically had relatively low levels of body fat; an almost universal feature among non-westernized hunter-gatherers.
Reference:
Poppitt, S.D. et al. (2008). Postprandial response of adiponectin, interleukin-6, tumor necrosis factor-α, and C-reactive protein to a high-fat dietary load. Nutrition, 24(4), 322-329.
Sunday, March 28, 2010
LDL, chylomicrons, HDL, and atherosclerosis: A lazy Sunday theory
Notes:
- This post is a joke, admittedly a weird one, which is why it is labeled “humor” and is filed under “Abstract humor”.
- I apologize for this spoiler. Some people probably like humor posts better if they do not know what they are in advance, but several others may think that reading a post like this is a waste of their time. If you are in the latter category, move on to another post! If not, here it goes …
Today I was spending some time under the sun, in one of the year’s 364 sunny days in Laredo, Texas. The goal was to see if I could obtain a precise count of the number of advanced glycation endproducts (a.k.a. AGEs) that would form as my skin was exposed to the sun’s damaging rays.
Then I read a post by Peter at Hyperlipid, and inspiration consumed me. A new theory was born regarding the interplay of LDL, chylomicrons, HDL, and atherosclerosis. By the way, Peter is a fat genius, by which I mean a genius regarding all fat issues – who happens to be thin.
A key observation forms the main pillar on which this new theory solidly rests:
The endothelium gaps, which let atherogenic particles enter into the forbidden area and do their damage, are around 25 nanometers in diameter. And what is the typical size of LDL particles? You guessed it, 25 nanometers in diameter! And guess what more, quite a few of the chylomicrons, another group of particles that would elicit immediate revulsion in any normal human being, are even smaller than 25 nanometers in diameter; those atherogenic pests!
So here is the theory, in a nutshell. A 500-page book will clearly be needed to discuss it in more detail.
The Devil created LDL particles to kill us all. But LDL particles were not such effective killers, because the Devil, trying to pack as much killer cholesterol into them, ended up making them too big! At 25 nanometers in diameter, on average, they basically had to squeeze their way into the forbidden area.
Since LDL particles were not doing a good enough job, the Devil also created chylomicrons, and those chaotic pests come in all sizes. In fact, it is well known that the word chylomicron has a Greek origin: chylo = killer, micron = particle (Deth & Disis, 1999; full reference at the end of this post).
And, needless to say, LDL particles and chylomicrons are fat particles that make the blood kind of taste and smell like butter, a toxic substance often fed to laboratory rats and known for its powerful carcinogenic properties among all living creatures except descendants of Vlad the Impaler. The latter has long been rumored to have been one of the Devil's best buddies, so no surprise there.
Michael the Archangel, who dislikes the Devil, and usually takes a hands-on approach to dealing with those he dislikes, the Devil in particular, gave us HDL particles. If you have any doubts about Michael’s hands-on approach, check the picture below (from: Wikipedia), which clearly shows what Michael had already done to the Devil. And that was over a relatively minor disagreement.
And don’t think about trying to discredit this theory by asking why HDL particles are so small compared with LDL particles and chylomicrons! This is easy. For the same reason that David was small and Goliath big!
But those nasty particles, the LDLs and chylomicrons, weren't only two big bullies, they were two against one. HDL particles were doing a valiant job at fighting the damage done by the Devil’s two evil particles, but not quite enough to save everybody from atherosclerosis.
Michael cried foul, and threatened to give the Devil another lesson. God, seeing this, said: Michael, no, mankind must be given a choice! If men and women want to gorge on the fatty flesh of the beasts they savagely slaughter, let them sin and face the consequences.
And so it was.
This theory probably needs some adjustments and refinements based on analysis of refereed research, especially solid research supported by drug manufacturers, and consultation with the most interesting man in the world. But I am pretty confident it can, after adjustments and refinements, pass the test of time.
The only nagging problem is the Original Sin. To the best of my knowledge, it was not eating the fatty flesh of beasts. It was eating a very sweet apple …
Reference:
Deth, R., & Disis, M. (1999, Feb 31). The origins of killer lipids: An evolutionary-theological perspective. The Lipid Review, 123(7), 77-66.
- This post is a joke, admittedly a weird one, which is why it is labeled “humor” and is filed under “Abstract humor”.
- I apologize for this spoiler. Some people probably like humor posts better if they do not know what they are in advance, but several others may think that reading a post like this is a waste of their time. If you are in the latter category, move on to another post! If not, here it goes …
***
Today I was spending some time under the sun, in one of the year’s 364 sunny days in Laredo, Texas. The goal was to see if I could obtain a precise count of the number of advanced glycation endproducts (a.k.a. AGEs) that would form as my skin was exposed to the sun’s damaging rays.
Then I read a post by Peter at Hyperlipid, and inspiration consumed me. A new theory was born regarding the interplay of LDL, chylomicrons, HDL, and atherosclerosis. By the way, Peter is a fat genius, by which I mean a genius regarding all fat issues – who happens to be thin.
A key observation forms the main pillar on which this new theory solidly rests:
The endothelium gaps, which let atherogenic particles enter into the forbidden area and do their damage, are around 25 nanometers in diameter. And what is the typical size of LDL particles? You guessed it, 25 nanometers in diameter! And guess what more, quite a few of the chylomicrons, another group of particles that would elicit immediate revulsion in any normal human being, are even smaller than 25 nanometers in diameter; those atherogenic pests!
So here is the theory, in a nutshell. A 500-page book will clearly be needed to discuss it in more detail.
The Devil created LDL particles to kill us all. But LDL particles were not such effective killers, because the Devil, trying to pack as much killer cholesterol into them, ended up making them too big! At 25 nanometers in diameter, on average, they basically had to squeeze their way into the forbidden area.
Since LDL particles were not doing a good enough job, the Devil also created chylomicrons, and those chaotic pests come in all sizes. In fact, it is well known that the word chylomicron has a Greek origin: chylo = killer, micron = particle (Deth & Disis, 1999; full reference at the end of this post).
And, needless to say, LDL particles and chylomicrons are fat particles that make the blood kind of taste and smell like butter, a toxic substance often fed to laboratory rats and known for its powerful carcinogenic properties among all living creatures except descendants of Vlad the Impaler. The latter has long been rumored to have been one of the Devil's best buddies, so no surprise there.
Michael the Archangel, who dislikes the Devil, and usually takes a hands-on approach to dealing with those he dislikes, the Devil in particular, gave us HDL particles. If you have any doubts about Michael’s hands-on approach, check the picture below (from: Wikipedia), which clearly shows what Michael had already done to the Devil. And that was over a relatively minor disagreement.
And don’t think about trying to discredit this theory by asking why HDL particles are so small compared with LDL particles and chylomicrons! This is easy. For the same reason that David was small and Goliath big!
But those nasty particles, the LDLs and chylomicrons, weren't only two big bullies, they were two against one. HDL particles were doing a valiant job at fighting the damage done by the Devil’s two evil particles, but not quite enough to save everybody from atherosclerosis.
Michael cried foul, and threatened to give the Devil another lesson. God, seeing this, said: Michael, no, mankind must be given a choice! If men and women want to gorge on the fatty flesh of the beasts they savagely slaughter, let them sin and face the consequences.
And so it was.
This theory probably needs some adjustments and refinements based on analysis of refereed research, especially solid research supported by drug manufacturers, and consultation with the most interesting man in the world. But I am pretty confident it can, after adjustments and refinements, pass the test of time.
The only nagging problem is the Original Sin. To the best of my knowledge, it was not eating the fatty flesh of beasts. It was eating a very sweet apple …
Reference:
Deth, R., & Disis, M. (1999, Feb 31). The origins of killer lipids: An evolutionary-theological perspective. The Lipid Review, 123(7), 77-66.
Friday, March 26, 2010
A trip to Europe: Some health-related routines and observations
Every year I travel to Europe on business, normally once or twice a year. These trips usually involve meetings with engineers, researchers, and project managers from various European countries; often 5 to 10 countries are represented.
Here are some of my notes on a recent trip to Europe. In this trip I spent time in two cities: Amsterdam, Netherlands and Antwerp, Belgium. Below is a set of the photos I took in Antwerp, of a statue depicting the roman soldier Silvius Brabo holding the severed hand of the giant Druon Antigoon.
According to legend Druon Antigoon had terrorized and extorted the people of Antwerp, cutting off the hands of several people and throwing them in the nearby Scheldt River, until the brave Silvius Brabo came into the scene and not only cut off the giant’s hand but also killed him.
This legend has probably been concocted toward the end of the Roman Empire, largely by the Romans, who first established Antwerp as a Roman outpost.
After this small digression, here are some health-related routines that I followed during this trip, and some of my main observations regarding diet and health issues.
On the plane:
- The meals were a festival of hyperglycemic and pro-inflammatory refined carbohydrates, unhealthy vegetable oils, and sugars – white bread, pasta, various sweets, pretzels, chips loaded with supposedly healthy omega 6 fats, margarine etc. I skipped all of the snacks and one of the meals, the breakfast. At the main meal of each flight I ate only meat, veggies, and some of the fruits.
- The flights over and back were very comfortable since I was water-fasting most of the time. Not a hint of indigestion or abdominal discomfort of any kind. These were 9 to 10 hour flights, from Houston to Amsterdam and back.
At business luncheons:
- The idea of having a sandwich for lunch seems to be getting popular in Europe. At least I have been seeing that happening more and more often lately. At these sandwich luncheons, I ate only the content of some sandwiches (basically cold cuts, cheese and veggies), and left the bread slices untouched.
- Some people noticed that I was not eating bread. I told them about insulin, lectins etc. A few looked at me as though I was insane; others with a disapproving look – dontchano, the lipid hypothesis!? A notable exception was a German gentleman who said that Germans were too pragmatic not to notice that they were getting fat on low fat diets, and are now reverting back to their staple diet of meats, fish, vegetable stews, and cheese.
At restaurants for dinner:
- This was fairly easy. I ate basically fish or meat dishes with veggies, and enjoyed them a lot. I skipped the deserts; again much to the surprise of some of my European colleagues.
- Skipping the desserts seems to have helped me cope with jetlag a lot better than I usually do. On my second day in Europe I slept quite well, and was unusually rested on the next day.
At the hotel:
- The breakfast buffets were a mix of: (a) breads, pastries, sweetened cereals, sugary items, and fruits; and (b) meats (often cured), some fish, cheeses, eggs, nuts, and some veggies. There were also fruit juices. I had solid breakfasts with (b)-type items, with a few fruits added (cantaloupe and berries). I had regular coffee with cream and no sugar, and stayed away from fruit juices.
- I did not use soap, shampoo etc. at the hotel; just plain water. Occasionally the soap used in hotels is very caustic, or rich in other chemicals, causing rashes. I stuck with showers and had no baths, as sometimes the bathtubs are not properly cleaned after their last use.
- At the end of my trip I took a train from Antwerp to Amsterdam, and stayed at a hotel near the Schiphol Airport (which has its own train station) since my flight back to the U.S. was in the morning. I had dinner by myself at the hotel, which was easy. I stopped at a place called Food Village at the Airport (visible from the Airport’s main entrance) and bought a water bottle, a piece of Gouda cheese, a can of sardines, and a box of seaweed. That was a very good dinner, and cost me about 6 euros.
The outcomes for me:
- I had no hint of indigestion at all throughout the trip, in spite of eating way more cheese than I normally do. The cheese that I ate was natural, aged cheese, not the processed kind.
- I had no need for more or less use of the bathroom than I usually do, and remained “regular” throughout the trip. No sign of constipation at all.
- I had no body odor (at least none that I could notice), even though I used no soap. My hair was fine too; I used no shampoo or conditioner.
- Jet lag problems were less pronounced than they usually are when I travel to Europe. The time difference is about 7 hours from Texas. Usually, I tend to feel very sleepy in the afternoon and wide awake around 3 am. Not this time.
- In spite of not exercising for about 7 days, except for walking, I was able to lift slightly heavier weights at a workout the day after my return than I did before my trip.
- According to the scale, I lost 1 pound during this trip. I do not know whether this was body fat or just water. It is unlikely that there was any muscle loss.
From what I could see, Europeans are generally thinner than Americans (particularly Texans), and also seem to be healthier. None of the people I met, not one, was clearly obese. On the other hand, the majority seemed to be somewhat overweight.
My impression was that the Europeans consume lesser amounts of refined carbohydrates and sugars than Americans, on a weekly basis, even though they currently consume more of those items than they should, in my opinion.
Consumption of vegetable oils other than olive oil is also lower than in the U.S; consumption of butter and cheese seems to be a lot higher.
From my conversations with several people during this trip, it seemed that the health of Europeans, like that of their American counterparts, is strongly correlated with the extent to which they are overweight. The more body fat, the more common was to hear complaints about pain here or there, fatigue, degenerative diseases, or talk about surgeries.
Here are some of my notes on a recent trip to Europe. In this trip I spent time in two cities: Amsterdam, Netherlands and Antwerp, Belgium. Below is a set of the photos I took in Antwerp, of a statue depicting the roman soldier Silvius Brabo holding the severed hand of the giant Druon Antigoon.
According to legend Druon Antigoon had terrorized and extorted the people of Antwerp, cutting off the hands of several people and throwing them in the nearby Scheldt River, until the brave Silvius Brabo came into the scene and not only cut off the giant’s hand but also killed him.
This legend has probably been concocted toward the end of the Roman Empire, largely by the Romans, who first established Antwerp as a Roman outpost.
After this small digression, here are some health-related routines that I followed during this trip, and some of my main observations regarding diet and health issues.
On the plane:
- The meals were a festival of hyperglycemic and pro-inflammatory refined carbohydrates, unhealthy vegetable oils, and sugars – white bread, pasta, various sweets, pretzels, chips loaded with supposedly healthy omega 6 fats, margarine etc. I skipped all of the snacks and one of the meals, the breakfast. At the main meal of each flight I ate only meat, veggies, and some of the fruits.
- The flights over and back were very comfortable since I was water-fasting most of the time. Not a hint of indigestion or abdominal discomfort of any kind. These were 9 to 10 hour flights, from Houston to Amsterdam and back.
At business luncheons:
- The idea of having a sandwich for lunch seems to be getting popular in Europe. At least I have been seeing that happening more and more often lately. At these sandwich luncheons, I ate only the content of some sandwiches (basically cold cuts, cheese and veggies), and left the bread slices untouched.
- Some people noticed that I was not eating bread. I told them about insulin, lectins etc. A few looked at me as though I was insane; others with a disapproving look – dontchano, the lipid hypothesis!? A notable exception was a German gentleman who said that Germans were too pragmatic not to notice that they were getting fat on low fat diets, and are now reverting back to their staple diet of meats, fish, vegetable stews, and cheese.
At restaurants for dinner:
- This was fairly easy. I ate basically fish or meat dishes with veggies, and enjoyed them a lot. I skipped the deserts; again much to the surprise of some of my European colleagues.
- Skipping the desserts seems to have helped me cope with jetlag a lot better than I usually do. On my second day in Europe I slept quite well, and was unusually rested on the next day.
At the hotel:
- The breakfast buffets were a mix of: (a) breads, pastries, sweetened cereals, sugary items, and fruits; and (b) meats (often cured), some fish, cheeses, eggs, nuts, and some veggies. There were also fruit juices. I had solid breakfasts with (b)-type items, with a few fruits added (cantaloupe and berries). I had regular coffee with cream and no sugar, and stayed away from fruit juices.
- I did not use soap, shampoo etc. at the hotel; just plain water. Occasionally the soap used in hotels is very caustic, or rich in other chemicals, causing rashes. I stuck with showers and had no baths, as sometimes the bathtubs are not properly cleaned after their last use.
- At the end of my trip I took a train from Antwerp to Amsterdam, and stayed at a hotel near the Schiphol Airport (which has its own train station) since my flight back to the U.S. was in the morning. I had dinner by myself at the hotel, which was easy. I stopped at a place called Food Village at the Airport (visible from the Airport’s main entrance) and bought a water bottle, a piece of Gouda cheese, a can of sardines, and a box of seaweed. That was a very good dinner, and cost me about 6 euros.
The outcomes for me:
- I had no hint of indigestion at all throughout the trip, in spite of eating way more cheese than I normally do. The cheese that I ate was natural, aged cheese, not the processed kind.
- I had no need for more or less use of the bathroom than I usually do, and remained “regular” throughout the trip. No sign of constipation at all.
- I had no body odor (at least none that I could notice), even though I used no soap. My hair was fine too; I used no shampoo or conditioner.
- Jet lag problems were less pronounced than they usually are when I travel to Europe. The time difference is about 7 hours from Texas. Usually, I tend to feel very sleepy in the afternoon and wide awake around 3 am. Not this time.
- In spite of not exercising for about 7 days, except for walking, I was able to lift slightly heavier weights at a workout the day after my return than I did before my trip.
- According to the scale, I lost 1 pound during this trip. I do not know whether this was body fat or just water. It is unlikely that there was any muscle loss.
From what I could see, Europeans are generally thinner than Americans (particularly Texans), and also seem to be healthier. None of the people I met, not one, was clearly obese. On the other hand, the majority seemed to be somewhat overweight.
My impression was that the Europeans consume lesser amounts of refined carbohydrates and sugars than Americans, on a weekly basis, even though they currently consume more of those items than they should, in my opinion.
Consumption of vegetable oils other than olive oil is also lower than in the U.S; consumption of butter and cheese seems to be a lot higher.
From my conversations with several people during this trip, it seemed that the health of Europeans, like that of their American counterparts, is strongly correlated with the extent to which they are overweight. The more body fat, the more common was to hear complaints about pain here or there, fatigue, degenerative diseases, or talk about surgeries.
Labels:
body fat,
cheese,
Europe,
my experience,
travel
Low-carb diets and dehydration
It is well known that dehydration is a potential adverse effect of a ketogenic diet, which is one higher in fat with adequate protein and lower in carbohydrates.
Nutritionists should be watchful, in particular, of those who use ketogenic diets as therapy for certain conditions such as epilepsy and type 2 diabetes.
A study in epileptic children on ketogenic diets, for example, found dehydration to be the "most common early-onset compllication"and higher in those who fasted (1-2). The dehydration could be partly blamed on the incidence of GI tract adverse effects (1).
When treating those with type 2 diabetes with a ketogenic diet, it is advisable to instruct drinking up to eight 8 oz. glasses of water daily. There may also be need for adjusting those recommendations if certain medications were used such as diuretics.
According to the researchers who performed an intervention trial on those with type 2 diabetes and a ketogenic diet that resulted in a few adverse effects, the following was concluded: "Until we learn more about using low carbohydrate diets, medical monitoring for hypoglycemia, dehydration, and electrolyte abnormalities is imperative in patients taking diabetes or diuretic medications" (1).
The lower carbs can have a diuretic effect on the body, which should lead clinicians to be aware and make recommendations for increased water intake as necessary.
References
2. Kang HC, Chung da E, Kim DW, Kim HD. Epilepsia 2004;45:1116-1123. Available at: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1198735/?tool=pmcentrez
Labels:
nutr therap
Kidneys: Animal vs Veggie Protein
I was curious to know what it is about animal protein in general that would affect kidneys more than vegetable protein. So I went searching for a study.
There was a human intervention trial from the Dept of Internal Medicine in Texas that I found, which had evaluated animal protein-rich diet on kidney stones and calcium. The study took 15 subjects and fed them either vegetable protein, vegetable and egg protein or animal protein for 12 days in three different periods (1). What the study found was that the animal protein diet "conferred an increased risk for uric acid stones" but a lesser risk than the vegetarian diet for "calcium oxalate or calcium phosphate stones" (1).
Because my question really wasn't sufficiently answered by this study, I decided to pursue what National Kidney Foundation had to say. Finally, I found a publication they put out referencing nutrition and speaking to vegetarian diets in which they basically state that the veggie diets aren't "rich in higher quality protein" (2), but that also that the best sources of vegetarian protein may be ones lower in potassium and phosphorus depending on kidney dysfunction.
At best, the main focus on kidney health is a balance between protein and carbs because too few leads to more protein break down as well as protein with sodium (lower is better), phosphorus (lower is better), calcium, potassium (sometimes higher, sometimes low is better) and, of course, water amounts for keeping kidneys functioning well (2).
References
1. Breslau NA, Brinkley L, Hill KD, Pak, CY. J Clin Endocrinol Metab. 1988 Jan;66(1):140-6. Available at: http://www.ncbi.nlm.nih.gov/pubmed/2826524
2. National Kidney Foundation. Nutrition and Early Kidney Disease. Available at: http://www.kidney.org/atoz/pdf/NutriKidFail_Stage1-4.pdf
Labels:
nutr therap
Why Evidence-based Nutrition
As a result of my profession in science communications, it is a fact of life that I come in to work to find 1-2 papers to read every morning on my desk. I must read an average of between 10 new scientific papers weekly. They can range from culture studies, animal studies, human clinical trials, epidemiological studies, meta-analyses or simply review articles.
As a writer who specializes in topics of nutrition, I am continually faced with the labor of assessing just how “big” the news coming from the study really is, whether or not it merits more attention by our research and sciences team, and whether or not we should communicate it to the public.
If I had any special talent for pointing out flaws or problems in studies, I would be thrilled. I don’t. Not at all. Lucky for me, however, I work with a few knowledgeable scientists with a keen awareness for what’s hot and what’s definitely not.
I doubt that many of my own colleagues share the same luxury that I have for being able to pass a study by an experienced nutritionist to help me place it in proper perspective for our audiences. This is simply evident by an Internet search for nutrition articles and a judgment of how other health writers handle their material.
Relying on experts to sift through the journals has been a unique experience, one that has been inspiring—which is why I now have hopes of ultimately gaining expertise of evidence-based nutrition (EBN) myself. EBN is simply true science and research, after all, and it informs decisions and practice.
It is my view that nutrition is a young science that is maturing quickly. I share a similar positive optimism for the field as Walter Willet, who has written of a merge of nutritional sciences with epidemiology to provide greater knowledge more quickly (1).
I follow with Willet’s assertion that nutritional research approaches are improving (that it won’t take us 100 years to discover flaws in dietary recommendations such as partially hydrogenated oils, for example(1)), and my interest is piqued in learning, as I would expect, that the study of genomics will further influence the future of nutrition.
While evidence-based nutrition and medicine may appear controversial to a few, I cannot see any other way for me, as I long to live in a world where science and statistics (even if we don’t “get” them) govern our understanding, not our often-flawed personal judgments.
I welcome the new process of nutritional epidemiology referenced by Willet that he expects will provide “vast and unprecedented information” (1). For that matter, I expect to be intensely studying as continual information appears over the next decade or so.
To achieve what Trisha Greenhalgh advises in her wonderful primer on evidence-based medicine, How to Read a Paper, it is my expectation to come away with the ability “not only to read papers, but also to read the right papers at the right time” (2) to best guide my decision making.
References
1. Willet WC. Nutritional epidemiology issues in chronic disease at the turn of the century. Epidemiol Rev. 2000;22(1):85-86. Available at: http://epirev.oxfordjournals.org/cgi/reprint/22/1/82.pdf
2. Greenhalgh T. How To Read A Paper: The Basics of Evidence Based Medicine. Malden, MA: Blackwell, 2006, p. 2.
As a writer who specializes in topics of nutrition, I am continually faced with the labor of assessing just how “big” the news coming from the study really is, whether or not it merits more attention by our research and sciences team, and whether or not we should communicate it to the public.
If I had any special talent for pointing out flaws or problems in studies, I would be thrilled. I don’t. Not at all. Lucky for me, however, I work with a few knowledgeable scientists with a keen awareness for what’s hot and what’s definitely not.
I doubt that many of my own colleagues share the same luxury that I have for being able to pass a study by an experienced nutritionist to help me place it in proper perspective for our audiences. This is simply evident by an Internet search for nutrition articles and a judgment of how other health writers handle their material.
Relying on experts to sift through the journals has been a unique experience, one that has been inspiring—which is why I now have hopes of ultimately gaining expertise of evidence-based nutrition (EBN) myself. EBN is simply true science and research, after all, and it informs decisions and practice.
It is my view that nutrition is a young science that is maturing quickly. I share a similar positive optimism for the field as Walter Willet, who has written of a merge of nutritional sciences with epidemiology to provide greater knowledge more quickly (1).
I follow with Willet’s assertion that nutritional research approaches are improving (that it won’t take us 100 years to discover flaws in dietary recommendations such as partially hydrogenated oils, for example(1)), and my interest is piqued in learning, as I would expect, that the study of genomics will further influence the future of nutrition.
While evidence-based nutrition and medicine may appear controversial to a few, I cannot see any other way for me, as I long to live in a world where science and statistics (even if we don’t “get” them) govern our understanding, not our often-flawed personal judgments.
I welcome the new process of nutritional epidemiology referenced by Willet that he expects will provide “vast and unprecedented information” (1). For that matter, I expect to be intensely studying as continual information appears over the next decade or so.
To achieve what Trisha Greenhalgh advises in her wonderful primer on evidence-based medicine, How to Read a Paper, it is my expectation to come away with the ability “not only to read papers, but also to read the right papers at the right time” (2) to best guide my decision making.
References
1. Willet WC. Nutritional epidemiology issues in chronic disease at the turn of the century. Epidemiol Rev. 2000;22(1):85-86. Available at: http://epirev.oxfordjournals.org/cgi/reprint/22/1/82.pdf
2. Greenhalgh T. How To Read A Paper: The Basics of Evidence Based Medicine. Malden, MA: Blackwell, 2006, p. 2.
Thursday, March 25, 2010
How much water do I drink?
I've been perusing through Dr. Batmanghelidj's book Your Body's Many Cries for Water. Yes, I'm well aware that it does not entirely scientific and does have a few claims that could be regarded as sensationalism for water (excess cholesterol is a result of too little water intake, really?).
I was intrigued, however, at some of the references to the possibility of chronic dehydration as an influence on disease and the beginnings of cellular aging, which can fuel chronic disease.
Plus, anyway, I needed to write a paper on water.
So, of course, I had to ask myself, "How much water do you drink?"
So here goes my diet for today:
8am: 1 cup of green tea (with 1 yogurt/protein shake/fruit)
10am: 1 cup of yerba maté (a habit passed from Argentine mom)
12pm: 1 cup iced tea (with chicken salad lunch)
2pm: 1 shot espresso
4pm: 1 cup yerba maté
6pm: 1 glass red wine (with 1 cup lentil-asparagus soup dinner)
9pm: 1 cup green tea
(Plenty of liquid, but no straight glasses of purified H2O.)
I suppose that from a nutritional standpoint, it appears I did pretty OK for the day and plenty of antioxidants from fruit, veggies, tea, maté, coffee, and red wine. I am simply trying to stick to a relatively decent DASH eating plan.
Although I didn't feel dehydrated (I drank about 7 cups of liquid), given what I have now read about water I'll probably have to reconsider what I'm doing.
I'm especially alarmed at the possible effects of chronic caffeine diminishing ATP and alcohol's influence on vasopressin causing dehydration. (And here I thought the regular tea, coffee and occasional red wine were pretty OK habits.)
It does make sense to me that cells would best function when well-hydrated. After all, as stated in the materials, life began in water, or an ancient primordial swamp.
No doubt in my mind that given our origins from the sea that it's water intake that is truly necessary for entire body's proper function (along with a bit of salt).
As the water-relationship makes common sense to me, I can see how I might recommend it as integrative therapy in certain situations, although I would hang back from calling it "prevention" or "cure" of disease without some considerable evidence-based research.
I admit I had no idea something like a low-grade "chronic dehydration" existed and could exist despite food and liquid intake and affected directly by caffeine and alcohol.
It seems to me that, since water represents pretty much the starting point of nutrition (at least from a cell's and ancient fishapod ancestor's standpoint), the topic of water intake definitely should be part of all nutrition programs.
My thoughts,
Wednesday, March 24, 2010
More on the Harvard study on saturated versus polyunsaturated fats
This is a follow up on this post, which addressed the main argument put forth in a recent BBC article. The BBC article argued that people should replace saturated with polyunsaturated fats to reduce their risk of heart disease.
Let us take a look at the actual Harvard study itself (i.e., the study discussed in the BBC article). The Harvard study is linked here.
This post, by Stephan Guyenet, already pointed out several problems with the study. Stephan actually reviewed the studies used in the meta-analysis, and also some that were excluded in the meta-analysis and that he believes should have been included.
Here are a few other problems, in addition to the ones already pointed out by Stephan:
One thing that looks suspicious about this Harvard meta-analysis study is that they say that: “Statistical evidence for substantial between-study heterogeneity was not present (Q-statistic p = 0.13; I2 = 37%).”
A meta-analysis is a study that essentially summarizes, in a statistically sophisticated way, a bunch of other studies (the “sourced” studies). Too much between-study heterogeneity (i.e., widely disparate results among sourced studies) is undesirable, because it can bias the results.
The problem is similar to that of trying to summarize net worth figures (e.g., by calculating their average) in a middle class neighborhood that happens to have a few billionaires living in it. The heterogeneity in wealth may lead to a wildly overestimated average.
Now, we know that p values go down with sample size, and are usually high with small samples unless the effect measured by the statistic is very strong, regardless of the statistic used.
Well, with a sample of only 8 studies, their p value (associated with the Q statistic) is close to being significant at the 0.05 level!
If this sample of sourced studies were a little higher (say, 20), there would be significant between-study heterogeneity, which would call the meta-analysis into question. This is a big problem, since a good meta-analysis is expected to include a large number of studies (e.g., greater than 100), and this one included only 8 studies.
Moreover, to the best of my knowledge, the Q statistic is not very reliable when used with small samples, due to its low power as a test of heterogeneity. This makes the p value reported even more problematic.
Finally, the sourced study with the largest sample (n = 9,057; thus possibly the most credible), indicated as “Minnesota CS” on Figure 2 of the Harvard study, found increased risk of heart disease associated with increased consumption of polyunsaturated fats and reduced consumption of saturated fats.
Reference:
Mozaffarian, D., Micha, R., & Wallace, S. (2010). Effects on Coronary Heart Disease of Increasing Polyunsaturated Fat in Place of Saturated Fat: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. PLoS Med., 7(3): e1000252. doi: 10.1371/journal.pmed.1000252.
Let us take a look at the actual Harvard study itself (i.e., the study discussed in the BBC article). The Harvard study is linked here.
This post, by Stephan Guyenet, already pointed out several problems with the study. Stephan actually reviewed the studies used in the meta-analysis, and also some that were excluded in the meta-analysis and that he believes should have been included.
Here are a few other problems, in addition to the ones already pointed out by Stephan:
One thing that looks suspicious about this Harvard meta-analysis study is that they say that: “Statistical evidence for substantial between-study heterogeneity was not present (Q-statistic p = 0.13; I2 = 37%).”
A meta-analysis is a study that essentially summarizes, in a statistically sophisticated way, a bunch of other studies (the “sourced” studies). Too much between-study heterogeneity (i.e., widely disparate results among sourced studies) is undesirable, because it can bias the results.
The problem is similar to that of trying to summarize net worth figures (e.g., by calculating their average) in a middle class neighborhood that happens to have a few billionaires living in it. The heterogeneity in wealth may lead to a wildly overestimated average.
Now, we know that p values go down with sample size, and are usually high with small samples unless the effect measured by the statistic is very strong, regardless of the statistic used.
Well, with a sample of only 8 studies, their p value (associated with the Q statistic) is close to being significant at the 0.05 level!
If this sample of sourced studies were a little higher (say, 20), there would be significant between-study heterogeneity, which would call the meta-analysis into question. This is a big problem, since a good meta-analysis is expected to include a large number of studies (e.g., greater than 100), and this one included only 8 studies.
Moreover, to the best of my knowledge, the Q statistic is not very reliable when used with small samples, due to its low power as a test of heterogeneity. This makes the p value reported even more problematic.
Finally, the sourced study with the largest sample (n = 9,057; thus possibly the most credible), indicated as “Minnesota CS” on Figure 2 of the Harvard study, found increased risk of heart disease associated with increased consumption of polyunsaturated fats and reduced consumption of saturated fats.
Reference:
Mozaffarian, D., Micha, R., & Wallace, S. (2010). Effects on Coronary Heart Disease of Increasing Polyunsaturated Fat in Place of Saturated Fat: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. PLoS Med., 7(3): e1000252. doi: 10.1371/journal.pmed.1000252.
Tuesday, March 23, 2010
BBC article's advice: Replace saturated with polyunsaturated fats
The BBC article is here. It is based on meta-analysis of eight previous studies conducted by Harvard researchers, which the article states cover more than 13,000 people. The article also says that: “… [saturated] fats raise the levels of bad cholesterol that block the arteries to the heart.” They are of course referring to LDL cholesterol as the "bad cholesterol".
Sourcing bias is a notorious problem with meta-analyses (i.e., the choice of studies to use in a meta-analysis). Another problem is that you cannot tell what the studies sourced controlled for. Consider a study that compares health markers for smokers and non-smokers, where the smokers eat more saturated fat than the non-smokers. This study may confuse the effect of smoking with that of saturated fat consumption. To be reliable, the study must analyze the effect of saturated fat consumption, controlling for smoking habits.
There are other statistical issues to be considered in meta-analyses. For example, some of the sourced studies may take nonlinear relationships into consideration and others not. In multivariate analysis studies, nonlinearity may lead to significantly different results from those obtained through more conventional linear analyses.
Finally, reaching misleading results with sound statistical analyses is not that hard. As my age went from 1 to 20 years, my weight was strongly correlated with the price of gasoline. Yet, neither my weight caused the price of gasoline, nor the other way around. When you look at an individual study, not a meta-analysis, you can at least try to identify the possible sources of bias and mistakes.
Having said that, a solid refutation of the main argument in the article can be made from many angles. Here is a simple refutation based on what I would call the “HDL cholesterol angle”, with links to posts and various refereed publications:
- Increasing HDL cholesterol levels, especially beyond 60 mg/dl, dramatically decreases the risk of heart disease; and this is an almost universal effect in humans. This reduction in risk occurs even for people who suffer from diabetes and familial hypercholesterolemia. The latter is a genetic condition that is associated with very elevated LDL cholesterol and that is rare, typically afflicting 1 in 500 people in its heterozygous (and most common) form.
- Increasing consumption of saturated fats (present in: lard, fatty meat, coconut oil) and dietary cholesterol (from: fish, organ meats, eggs), while decreasing consumption of refined carbohydrates (e.g., pasta, white bread) and sugars (e.g., table sugar, high fructose corn syrup), significantly increases HDL cholesterol for the vast majority of people. Neither omega-6 nor omega-3 polyunsaturated fats lead to the same results. Omega-3 fats do reduce triglycerides, and increase HDL somewhat, but their effect on HDL pales in comparison with that of saturated fats. Excessive consumption of omega-6 fats is associated with chronic inflammation and related health problems.
- With the exception of cases involving familial hypercholesterolemia, there is no conclusive evidence that LDL cholesterol levels are associated with heart disease. Two widely used online calculators of risk of heart disease, based on the Framingham Heart Study and the Reynold Risk Score, do not even ask for LDL cholesterol levels to estimate risk. And that is not because they calculate LDL cholesterol based on other figures; they do not ask for VLDL cholesterol or triglycerides either.
After reading the BBC article again, it is clear that they are re-stating, in general terms, Rudolph Virchow’s mid-1800s lipid hypothesis. And they do so as if it was big news!
Sourcing bias is a notorious problem with meta-analyses (i.e., the choice of studies to use in a meta-analysis). Another problem is that you cannot tell what the studies sourced controlled for. Consider a study that compares health markers for smokers and non-smokers, where the smokers eat more saturated fat than the non-smokers. This study may confuse the effect of smoking with that of saturated fat consumption. To be reliable, the study must analyze the effect of saturated fat consumption, controlling for smoking habits.
There are other statistical issues to be considered in meta-analyses. For example, some of the sourced studies may take nonlinear relationships into consideration and others not. In multivariate analysis studies, nonlinearity may lead to significantly different results from those obtained through more conventional linear analyses.
Finally, reaching misleading results with sound statistical analyses is not that hard. As my age went from 1 to 20 years, my weight was strongly correlated with the price of gasoline. Yet, neither my weight caused the price of gasoline, nor the other way around. When you look at an individual study, not a meta-analysis, you can at least try to identify the possible sources of bias and mistakes.
Having said that, a solid refutation of the main argument in the article can be made from many angles. Here is a simple refutation based on what I would call the “HDL cholesterol angle”, with links to posts and various refereed publications:
- Increasing HDL cholesterol levels, especially beyond 60 mg/dl, dramatically decreases the risk of heart disease; and this is an almost universal effect in humans. This reduction in risk occurs even for people who suffer from diabetes and familial hypercholesterolemia. The latter is a genetic condition that is associated with very elevated LDL cholesterol and that is rare, typically afflicting 1 in 500 people in its heterozygous (and most common) form.
- Increasing consumption of saturated fats (present in: lard, fatty meat, coconut oil) and dietary cholesterol (from: fish, organ meats, eggs), while decreasing consumption of refined carbohydrates (e.g., pasta, white bread) and sugars (e.g., table sugar, high fructose corn syrup), significantly increases HDL cholesterol for the vast majority of people. Neither omega-6 nor omega-3 polyunsaturated fats lead to the same results. Omega-3 fats do reduce triglycerides, and increase HDL somewhat, but their effect on HDL pales in comparison with that of saturated fats. Excessive consumption of omega-6 fats is associated with chronic inflammation and related health problems.
- With the exception of cases involving familial hypercholesterolemia, there is no conclusive evidence that LDL cholesterol levels are associated with heart disease. Two widely used online calculators of risk of heart disease, based on the Framingham Heart Study and the Reynold Risk Score, do not even ask for LDL cholesterol levels to estimate risk. And that is not because they calculate LDL cholesterol based on other figures; they do not ask for VLDL cholesterol or triglycerides either.
After reading the BBC article again, it is clear that they are re-stating, in general terms, Rudolph Virchow’s mid-1800s lipid hypothesis. And they do so as if it was big news!
Monday, March 22, 2010
PepsiCo to reduce sugar and fat in products
I guess PepsiCo is moving ahead of the competition, but in a snail pace and in a very, very politically correct way. Will this help in any way? I doubt. It is just too little, too late. See article here.
The article states that:
The bottom line is that, if you want to improve your health, you should generally avoid any food or liquid that is highly industrialized.
Maybe PepsiCo should add unprocessed coconut water to their portfolio of drinks.
The article states that:
The company also set two goals for the next 10 years: to cut the average added sugar per serving by 25 percent and saturated fat per serving by 15 percent, in addition to adding more whole grains, fruits, vegetables and low-fat dairy into its array of products.While it is nice to see more of a focus on sugar than on saturated fat, I would have preferred to see something like this:
The company also set two goals for the next 5 years: to cut the average added sugar per serving by 95 percent and increase saturated fat per serving by 50 percent, in addition to adding more vegetables and full-fat dairy into its array of products.What would happen? Well, Indra Nooyi is a very smart CEO, and the company has many competent people. They know that they would probably lose enough customers to go out of business … or become the Apple of their industry.
The bottom line is that, if you want to improve your health, you should generally avoid any food or liquid that is highly industrialized.
Maybe PepsiCo should add unprocessed coconut water to their portfolio of drinks.
Friday, March 19, 2010
Online calculators to assess cardiovascular disease risk: No LDL needed
Researchers can build mathematical equations (sometimes referred to as structural equations) that predict health outcomes based on health factors. Those mathematical equations can then be used in online calculators.
This link takes you to a government-sponsored calculator based on the Framingham Heart Study. It estimates 10-year risk for “hard” coronary heart disease outcomes (myocardial infarction and coronary death).
As you will notice, the link above does not take family history of disease into consideration. A different risk calculator, linked here, estimates a risk score called the Reynold Risk Score. It takes hsCRP (high sensitivity C-reactive protein, an inflammation marker) and family history in addition to the Framingham parameters in its risk score calculation.
Neither calculator asks for LDL cholesterol levels. I wonder why.
This link takes you to a government-sponsored calculator based on the Framingham Heart Study. It estimates 10-year risk for “hard” coronary heart disease outcomes (myocardial infarction and coronary death).
As you will notice, the link above does not take family history of disease into consideration. A different risk calculator, linked here, estimates a risk score called the Reynold Risk Score. It takes hsCRP (high sensitivity C-reactive protein, an inflammation marker) and family history in addition to the Framingham parameters in its risk score calculation.
Neither calculator asks for LDL cholesterol levels. I wonder why.
Standard deviation is not the same as range of variation
Often research results are expressed in means and standard deviations. For example, in the study reviewed in this post, it is stated that the weight of participants in a 12-week weight loss study varied from: 87.9 plus or minus 15.4 kg (at baseline, or before the 12-week intervention) to 81.7 plus or minus 16.2 kg (after the 12-week intervention).
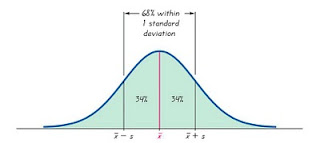
The 87.9 and 81.7 are the average weights (a.k.a. “mean” weights), in kilograms, before and after the 12-week intervention. However, the 15.4 and 16.2 are NOT the range of variation in weights around the means before and after 12-week intervention. They are actually the ranges around the means encompassing approximately 68 percent of all of the values measured (see figure below, from www.electrical-res.com).
In the figure above, the minus and plus 15.4 and 16.2 values would be the “mean(x) – s” and “mean(x) + s” points on the horizontal axis of histograms of weights plotted before and after the 12-week intervention. This assumes that the distributions of weights are normal, or quasi-normal (i.e., similar to a bell-shaped, or normal, curve); a common assumption in this type of research.
The larger the standard deviation, the wider is the variation in the measures, and the flatter is the associated histogram (the bell-shaped curve). This property has a number of interesting implications, some of which will be discussed in other posts.
Sometimes another measure of dispersion, the variance, is reported instead of the standard deviation. The variance is the standard deviation squared.
The reason why standard deviations are reported instead of ranges of variation is that outliers (unusually high or low values) can dramatically widen the ranges. The standard deviation coefficient is much less sensitive to outliers.
The 87.9 and 81.7 are the average weights (a.k.a. “mean” weights), in kilograms, before and after the 12-week intervention. However, the 15.4 and 16.2 are NOT the range of variation in weights around the means before and after 12-week intervention. They are actually the ranges around the means encompassing approximately 68 percent of all of the values measured (see figure below, from www.electrical-res.com).
In the figure above, the minus and plus 15.4 and 16.2 values would be the “mean(x) – s” and “mean(x) + s” points on the horizontal axis of histograms of weights plotted before and after the 12-week intervention. This assumes that the distributions of weights are normal, or quasi-normal (i.e., similar to a bell-shaped, or normal, curve); a common assumption in this type of research.
The larger the standard deviation, the wider is the variation in the measures, and the flatter is the associated histogram (the bell-shaped curve). This property has a number of interesting implications, some of which will be discussed in other posts.
Sometimes another measure of dispersion, the variance, is reported instead of the standard deviation. The variance is the standard deviation squared.
The reason why standard deviations are reported instead of ranges of variation is that outliers (unusually high or low values) can dramatically widen the ranges. The standard deviation coefficient is much less sensitive to outliers.
Monday, March 15, 2010
What's the most dangerous item on a fast food menu?
When I first saw the movie Super Size MeI was first pretty shocked that someone would actually risk his own body this way. Then, I was shocked at how quickly this guy was able to gain weight. This may simply be because I don't tend to gain any weight even after stuffing myself day after day. Of course, I've never tried to stuff myself with McDonald's day after day. Maybe that would do it. It did for this guy. And it does for our children. Sure opened my eyes.
What's the most dangerous item on the fast food menu?
I remember a time when I was younger I would go off with my grandpa to Burger King. He'd say, "Let's get you a Whopper. They're only a buck." I'd gush with enthusiasm. He'd buy me one. He'd buy himself too.
My grandpa died of heart disease. I blame it on those Whoppers. I blame them because they're cheap and because the name itself, like the Big Mac, suggest that you're getting a lot of meat for your money. What you're really getting is a gimmick and a lot of saturated and trans fat. I have no doubt that Burger King Whoppers (they ate them all the time) are what killed both my grandfather and my grandmother.
What's the most dangerous item on the fast food menu?
I remember a time when I was younger I would go off with my grandpa to Burger King. He'd say, "Let's get you a Whopper. They're only a buck." I'd gush with enthusiasm. He'd buy me one. He'd buy himself too.
My grandpa died of heart disease. I blame it on those Whoppers. I blame them because they're cheap and because the name itself, like the Big Mac, suggest that you're getting a lot of meat for your money. What you're really getting is a gimmick and a lot of saturated and trans fat. I have no doubt that Burger King Whoppers (they ate them all the time) are what killed both my grandfather and my grandmother.
Labels:
nutr therap
Why Statins May Require You Take Extra CoQ10 and Vitamin E
Statins are drugs used to lower cholesterol by blocking cholesterol synthesis in the liver (1). By lowering total and LDL cholesterol, in effect, they help lower risk of heart disease and death (1). The most commonly known statin drugs are simvastatin (Zocor), lovastatin (Mevacor), pravastatin (Pravachol), and rosuvastatin (Crestor).
Currently, it is theorized that as statins block cholesterol synthesis, they also block synthesis of coenzyme Q10 (2). This is unfortunate because coenzyme Q10 plays a key role in the mitochondria in the electron transport chain, as an antioxidant and as a regenerator of vitamin E (3).
Statin therapy, then, could potentially lead to deficiencies of both coenzyme Q10 and, possibly, increase the need for vitamin E in cells (4). It has been theorized that deficiencies in both coenzyme Q10 and vitamin E are why statins cause statin-related muscle pain and statin-related myopathy (3-4).
References
1. LaRosa JC, He J, Vupputuri S. Effect of statins on risk of coronary disease: a meta-analysis of randomized controlled trials. JAMA. 1999 Dec 22-29;282(24):2340-6. Available at: http://www.ncbi.nlm.nih.gov/pubmed/10612322
2. Schaars CF, Stalenhoef AF. Effects of ubiquinone (coenzyme Q10) on myopathy in statin users. Curr Opin Lipidol. 2008 Dec;19(6):553-7.
3. Gropper SS, Smith JL, Groff JL. Advanced Nutrition and Human Metabolism. Belmont, CA: Thomson Wadsworth, 2009.
4. Galli F, Iuliano L. Do statins cause myopathy by lowering vitamin E levels? Med Hypotheses. 2010 Apr;74(4):707-709. Epub 2009 Nov 6.
Currently, it is theorized that as statins block cholesterol synthesis, they also block synthesis of coenzyme Q10 (2). This is unfortunate because coenzyme Q10 plays a key role in the mitochondria in the electron transport chain, as an antioxidant and as a regenerator of vitamin E (3).
Statin therapy, then, could potentially lead to deficiencies of both coenzyme Q10 and, possibly, increase the need for vitamin E in cells (4). It has been theorized that deficiencies in both coenzyme Q10 and vitamin E are why statins cause statin-related muscle pain and statin-related myopathy (3-4).
References
1. LaRosa JC, He J, Vupputuri S. Effect of statins on risk of coronary disease: a meta-analysis of randomized controlled trials. JAMA. 1999 Dec 22-29;282(24):2340-6. Available at: http://www.ncbi.nlm.nih.gov/pubmed/10612322
2. Schaars CF, Stalenhoef AF. Effects of ubiquinone (coenzyme Q10) on myopathy in statin users. Curr Opin Lipidol. 2008 Dec;19(6):553-7.
3. Gropper SS, Smith JL, Groff JL. Advanced Nutrition and Human Metabolism. Belmont, CA: Thomson Wadsworth, 2009.
4. Galli F, Iuliano L. Do statins cause myopathy by lowering vitamin E levels? Med Hypotheses. 2010 Apr;74(4):707-709. Epub 2009 Nov 6.
Labels:
nutr therap
What are blood thinners and how do they work?
Blood thinners, or anticoagulants and antiplatelet agents, are drugs to thwart blood clotting of which could block flow of blood to your heart causing a heart attack or your brain causing a stroke.
Common anticoagulants are Coumadin, Warfarin and Heparin. It controls the rate in which clotting can occur and prevents them from forming inside blood vessels and the heart. It can also help prevent existing clots from enlarging.
Common antiplatelet agents are Aspirin, Plavix (clopidogrel bisulfate) and Ticlid (ticlopidene hydrochloride). As the name suggests, they keep platelets from aggregation to prevent possible clotting, specifically where an injury to a blood vessel may have occurred.
Blood thinners aren't associated with any specific nutrient deficiency, but are contraindicated taken with foods and supplements high in vitamin K1 (a clotting factor) or large amounts of vitamins E and C. They are also contraindicated with alcohol, certain herbs and teas, and other dietary agents that cause thinning of blood.
Reference
http://www.nlm.nih.gov/medlineplus/bloodthinners.html
Common anticoagulants are Coumadin, Warfarin and Heparin. It controls the rate in which clotting can occur and prevents them from forming inside blood vessels and the heart. It can also help prevent existing clots from enlarging.
Common antiplatelet agents are Aspirin, Plavix (clopidogrel bisulfate) and Ticlid (ticlopidene hydrochloride). As the name suggests, they keep platelets from aggregation to prevent possible clotting, specifically where an injury to a blood vessel may have occurred.
Blood thinners aren't associated with any specific nutrient deficiency, but are contraindicated taken with foods and supplements high in vitamin K1 (a clotting factor) or large amounts of vitamins E and C. They are also contraindicated with alcohol, certain herbs and teas, and other dietary agents that cause thinning of blood.
Reference
http://www.nlm.nih.gov/medlineplus/bloodthinners.html
Labels:
nutr therap
Sunday, March 14, 2010
Ketosis, methylglyoxal, and accelerated aging: Probably more fiction than fact
This is a follow up on this post. Just to recap, an interesting hypothesis has been around for quite some time about a possible negative effect of ketosis. This hypothesis argues that ketosis leads to the production of an organic compound called methylglyoxal, which is believed to be a powerful agent in the formation of advanced glycation endproducts (AGEs).
In vitro research, and research with animals (e.g., mice and cows), indeed suggests negative short-term effects of increased ketosis-induced methylglyoxal production. These studies typically deal with what appears to be severe ketosis, not the mild type induced in healthy people by very low carbohydrate diets.
However, the bulk of methylglyoxal is produced via glycolysis, a multi-step metabolic process that uses sugar to produce the body’s main energy currency – adenosine triphosphate (ATP). Ketosis is a state whereby ketones are used as a source of energy instead of glucose.
(Ketones also provide an energy source that is distinct from lipoprotein-bound fatty acids and albumin-bound free fat acids. Those fatty acids appear to be preferred vehicles for the use of dietary or body fat as a source of energy. Yet it seems that small amounts of ketones are almost always present in the blood, even if they do not show up in the urine.)
Thus it follows that ketosis is associated with reduced glycolysis and, consequently, reduced methylglyoxal production, since the bulk of this substance (i.e., methylglyoxal) is produced through glycolysis.
So, how can one argue that ketosis is “a recipe for accelerated AGEing”?
One guess is that ketosis is being confused with ketoacidosis, a pathological condition in which the level of circulating ketones can be as much as 40 to 80 times that found in ketosis. De Grey (2007) refers to “diabetic patients” when he talks about this possibility (i.e., the connection with accelerated AGEing), and ketoacidosis is an unfortunately common condition among those with uncontrolled diabetes.
A gentle body massage is relaxing, and thus health-promoting. Add 40 times to the pressure, and the massage will become a form of physical torture; certainly unhealthy. That does not mean that a gentle body massage is unhealthy.
Interestingly, ketoacidosis often happens together with hyperglycemia, so at least part of the damage associated with ketoacidosis is likely to be caused by high blood sugar levels. Ketosis, on the other hand, is not associated with hyperglycemia.
Finally, if ketosis led to accelerated AGEing to the same extent as, or worse than, chronic hyperglycemia does, where is the long-term evidence?
Since the late 1800s people have been experimenting with ketosis-inducing diets, and documenting the results. The Inuit and other groups have adopted ketosis-inducing diets for much longer, although evolution via selection might have played a role in these cases.
No one seems to have lived to be 150 years of age, but where are the reports of conditions akin to those caused by chronic hyperglycemia among the many that went “banting” in a more strict way since the late 1800s?
The arctic explorer Vilhjalmur Stefansson, who is reported to have lived much of his adult life in ketosis, died in 1962, in his early 80s. After reading about his life, few would disagree that he lived a rough life, with long periods without access to medical care. I doubt that Stefansson would have lived that long if he had suffered from untreated diabetes.
Severe ketosis, to the point of large amounts of ketones being present in the urine, may not be a natural state in which our Paleolithic ancestors lived most of the time. In modern humans, even a 24 h water fast, during an already low carbohydrate diet, may not induce ketosis of this type. Milder ketosis states, with slightly elevated concentrations of ketones showing up in blood tests, can be achieved much more easily.
In conclusion, the notion that ketosis causes accelerated aging to the same extent as chronic hyperglycemia seems more like fiction than fact.
Reference:
De Grey, A. (2007). Ending aging: The rejuvenation breakthroughs that could reverse human aging in our lifetime. New York: NY: St. Martin’s Press.
In vitro research, and research with animals (e.g., mice and cows), indeed suggests negative short-term effects of increased ketosis-induced methylglyoxal production. These studies typically deal with what appears to be severe ketosis, not the mild type induced in healthy people by very low carbohydrate diets.
However, the bulk of methylglyoxal is produced via glycolysis, a multi-step metabolic process that uses sugar to produce the body’s main energy currency – adenosine triphosphate (ATP). Ketosis is a state whereby ketones are used as a source of energy instead of glucose.
(Ketones also provide an energy source that is distinct from lipoprotein-bound fatty acids and albumin-bound free fat acids. Those fatty acids appear to be preferred vehicles for the use of dietary or body fat as a source of energy. Yet it seems that small amounts of ketones are almost always present in the blood, even if they do not show up in the urine.)
Thus it follows that ketosis is associated with reduced glycolysis and, consequently, reduced methylglyoxal production, since the bulk of this substance (i.e., methylglyoxal) is produced through glycolysis.
So, how can one argue that ketosis is “a recipe for accelerated AGEing”?
One guess is that ketosis is being confused with ketoacidosis, a pathological condition in which the level of circulating ketones can be as much as 40 to 80 times that found in ketosis. De Grey (2007) refers to “diabetic patients” when he talks about this possibility (i.e., the connection with accelerated AGEing), and ketoacidosis is an unfortunately common condition among those with uncontrolled diabetes.
A gentle body massage is relaxing, and thus health-promoting. Add 40 times to the pressure, and the massage will become a form of physical torture; certainly unhealthy. That does not mean that a gentle body massage is unhealthy.
Interestingly, ketoacidosis often happens together with hyperglycemia, so at least part of the damage associated with ketoacidosis is likely to be caused by high blood sugar levels. Ketosis, on the other hand, is not associated with hyperglycemia.
Finally, if ketosis led to accelerated AGEing to the same extent as, or worse than, chronic hyperglycemia does, where is the long-term evidence?
Since the late 1800s people have been experimenting with ketosis-inducing diets, and documenting the results. The Inuit and other groups have adopted ketosis-inducing diets for much longer, although evolution via selection might have played a role in these cases.
No one seems to have lived to be 150 years of age, but where are the reports of conditions akin to those caused by chronic hyperglycemia among the many that went “banting” in a more strict way since the late 1800s?
The arctic explorer Vilhjalmur Stefansson, who is reported to have lived much of his adult life in ketosis, died in 1962, in his early 80s. After reading about his life, few would disagree that he lived a rough life, with long periods without access to medical care. I doubt that Stefansson would have lived that long if he had suffered from untreated diabetes.
Severe ketosis, to the point of large amounts of ketones being present in the urine, may not be a natural state in which our Paleolithic ancestors lived most of the time. In modern humans, even a 24 h water fast, during an already low carbohydrate diet, may not induce ketosis of this type. Milder ketosis states, with slightly elevated concentrations of ketones showing up in blood tests, can be achieved much more easily.
In conclusion, the notion that ketosis causes accelerated aging to the same extent as chronic hyperglycemia seems more like fiction than fact.
Reference:
De Grey, A. (2007). Ending aging: The rejuvenation breakthroughs that could reverse human aging in our lifetime. New York: NY: St. Martin’s Press.
Thursday, March 11, 2010
Ketosis, methylglyoxal, and accelerated aging: Fact or fiction?
Ketosis is a state typically associated with very low carbohydrate diets, such as the Atkins diet. In this state, the liver produces ketones based on fat (body fat or dietary fat). Unlike fats, ketones are water soluble and used by many tissues (including brain tissues) as a source of energy.
Unlike glucose and lipoprotein-bound fats (in VLDL, for example), unused ketones cannot be converted back to substances that can be stored by the body. Thus excess ketones are eliminated in the urine; leading to their detection by various tests, e.g., Ketostix tests.
This elimination of unused ketones in the urine is one of the reasons why very low carbohydrate diets are believed to lead to enhanced body fat loss.
From an evolutionary perspective, one could argue that a ketosis state that involves the elimination of ketones in the urine is an inefficient and unnatural emergency mechanism. For our Paleolithic ancestors, dying of starvation was a much bigger problem than dying of obesity complications.
An interesting hypothesis has been around for quite some time about a possible negative effect of ketosis. It goes more or less like this. Ketosis leads to the production of an organic compound called methylglyoxal, which is believed to be a powerful agent of glycation (a misnomer; see note below).
Glycation is a process whereby sugar molecules “stick” to protein or fat molecules, impairing their function. Glycation leads to the formation of advanced glycation endproducts (AGEs), which appear to be associated with a host of diseases, including diabetes, and to be implicated in accelerated aging (or “ageing”, with British spelling).
In short: ketosis leads to the production of methylglyoxal, which leads to the formation of AGEs, which in turn cause diseases and accelerated aging.
Note: Since glycation refers to “sugar” molecules sticking to protein and fats, its use in the context of methylglyoxal is arguably incorrect. Methylglyoxal is not a sugar, but an aldehyde.
One of the strongest indictments of ketosis, in relation to methylglyoxal, is made in a fairly well referenced book by De Grey (2007); the full reference to the book is at the end of this post. De Grey’s book is about aging, and how to stop or at least delay it. Overall, it is an excellent book. Here is some relevant text, from page 173 of the book:
Sorry, but I need to consult with my guru before I post my answer.
Reference:
De Grey, A. (2007). Ending aging: The rejuvenation breakthroughs that could reverse human aging in our lifetime. New York: NY: St. Martin’s Press.
Unlike glucose and lipoprotein-bound fats (in VLDL, for example), unused ketones cannot be converted back to substances that can be stored by the body. Thus excess ketones are eliminated in the urine; leading to their detection by various tests, e.g., Ketostix tests.
This elimination of unused ketones in the urine is one of the reasons why very low carbohydrate diets are believed to lead to enhanced body fat loss.
From an evolutionary perspective, one could argue that a ketosis state that involves the elimination of ketones in the urine is an inefficient and unnatural emergency mechanism. For our Paleolithic ancestors, dying of starvation was a much bigger problem than dying of obesity complications.
An interesting hypothesis has been around for quite some time about a possible negative effect of ketosis. It goes more or less like this. Ketosis leads to the production of an organic compound called methylglyoxal, which is believed to be a powerful agent of glycation (a misnomer; see note below).
Glycation is a process whereby sugar molecules “stick” to protein or fat molecules, impairing their function. Glycation leads to the formation of advanced glycation endproducts (AGEs), which appear to be associated with a host of diseases, including diabetes, and to be implicated in accelerated aging (or “ageing”, with British spelling).
In short: ketosis leads to the production of methylglyoxal, which leads to the formation of AGEs, which in turn cause diseases and accelerated aging.
Note: Since glycation refers to “sugar” molecules sticking to protein and fats, its use in the context of methylglyoxal is arguably incorrect. Methylglyoxal is not a sugar, but an aldehyde.
One of the strongest indictments of ketosis, in relation to methylglyoxal, is made in a fairly well referenced book by De Grey (2007); the full reference to the book is at the end of this post. De Grey’s book is about aging, and how to stop or at least delay it. Overall, it is an excellent book. Here is some relevant text, from page 173 of the book:
… one established effect of very low-carbohydrate diets of the Atkins type is to bring down both triglyceride levels and the body’s total exposure to carbohydrates, so some advocates have hypothesized that these diets world reduce a person’s AGE burden. Unfortunately, it turns out that the metabolic state that these diets induce (the notorious “ketosis”) has the unfortunate side effect of causing a jump in the production of the oxoaldehyde methylglyoxal, a major precursor of AGEs that is also, ironically, produced within cells of diabetic patients when they are forced to take in more glucose than they can immediately process … methylglyoxal is far more chemically reactive than blood sugar (up to 40,000 times more reactive, in fact), and is known to cause wide-ranging damage in the body, of which AGE cross-links are but one example. This potentially makes the Atkins diet a recipe for accelerated AGEing …Is this notion that ketosis, through methylglyoxal, can cause accelerated aging fact or fiction?
Sorry, but I need to consult with my guru before I post my answer.
Reference:
De Grey, A. (2007). Ending aging: The rejuvenation breakthroughs that could reverse human aging in our lifetime. New York: NY: St. Martin’s Press.
Monday, March 8, 2010
Steamed gulf shrimp with vegetables
Few would argue against eating seafood several times a week, except in the case of seafood allergy. Shrimp is a very good option, especially if it is not farm raised.
100 g of shrimp will typically have 20 g of protein, and about 152 mg of cholesterol (this is good for your health). It will also have about 0.6 g of omega-3 fats, and 0.03 g of omega-6; an omega-3 to omega-6 ratio of about 20.
My wife prepared this steamed gulf shrimp with vegetables dish. And it was very, very delicious. Here is her recipe:
- Add a small amount of olive oil and water to a frying pan.
- Add 1 lb of wild-caught peeled gulf shrimp, cabbage, onion, and asparagus (or green beans, as in the photo).
- Cook in low heat for 15 minutes.
- Add spinach and cook in low heat for another 10 minutes.
- Turn off heat, season to taste while mixing; I suggest using garlic powder, cumin powder, and parsley flakes.
Peeled shrimp is usually farm raised, which does not have the same amount of omega-3, or the same ratio of omega-3 to omega-6, as wild-caught shrimp. This small “salad” gulf shrimp was an exception.
Check the package. If it doesn’t explicitly say “wild”, you are better off buying wild-caught shrimp and peeling it yourself. Shrimp peelers are sold in most supermarkets; the one I use looks like a Velociraptor claw.
100 g of shrimp will typically have 20 g of protein, and about 152 mg of cholesterol (this is good for your health). It will also have about 0.6 g of omega-3 fats, and 0.03 g of omega-6; an omega-3 to omega-6 ratio of about 20.
My wife prepared this steamed gulf shrimp with vegetables dish. And it was very, very delicious. Here is her recipe:
- Add a small amount of olive oil and water to a frying pan.
- Add 1 lb of wild-caught peeled gulf shrimp, cabbage, onion, and asparagus (or green beans, as in the photo).
- Cook in low heat for 15 minutes.
- Add spinach and cook in low heat for another 10 minutes.
- Turn off heat, season to taste while mixing; I suggest using garlic powder, cumin powder, and parsley flakes.
Peeled shrimp is usually farm raised, which does not have the same amount of omega-3, or the same ratio of omega-3 to omega-6, as wild-caught shrimp. This small “salad” gulf shrimp was an exception.
Check the package. If it doesn’t explicitly say “wild”, you are better off buying wild-caught shrimp and peeling it yourself. Shrimp peelers are sold in most supermarkets; the one I use looks like a Velociraptor claw.
Wednesday, March 3, 2010
Adiponectin and tumor necrosis factor-alpha levels after a high saturated fat meal
This is one of those interesting studies where the authors start with some pre-conceived assumptions and end up concluding something else, some way toward the opposite of what they assumed.
My final interpretation of the study results is a bit different though. It suggests that the results are actually the opposite of what the authors originally assumed.
The authors of the study (Poppitt et al., 2008; full reference at the end of this post) start by stating that since “… dietary fat is associated with increased lipid storage, weight gain, and obesity …” it is important to study the effect of dietary fat intake on the blood levels of certain substances that are associated with lipid disorders, weight gain and obesity.
In short, the authors start from the assumption that dietary fat is bad. By the way, this type of indictment of all fats is not very common these days. Usually saturated fat is the target.
Since dietary fat is assumed to be bad for us, that justifies the authors’ goal of studying the effect of dietary fat on certain hormones associated with bad health, including the body fat-secreted hormones adiponectin and tumor necrosis factor-alpha. Low levels of serum adiponectin, and elevated levels of tumor necrosis factor-alpha, are associated with various health complications.
In the study, a high-fat test meal with approximately 59 g of fat (71% of energy as fat) was given at breakfast on two occasions to 18 healthy and lean men. These men had, on average, 23 years of age, a 31-inch waist, and a body mass index of 22.9. In other words, they were young and fit.
Two fatty meal variations were used, one with a lot more saturated fat than the other. Their ratio of saturated:unsaturated fatty acids was 71:29 for the high saturated fat meal, and 55:45 for the other. The table below provides a more detailed picture of the fat composition of the meals. The authors refer to these meals as instances of “acute intake of dietary lipid”.
Lunch, snack and dinner meals were also served to the participants. Those meals were nearly fat-free, with 1 to 3 g of fat only; apparently to help the participants “recover” from the high fat meal. They included plenty of refined grains (e.g., pasta) and fruit juices. Way to go; give these folks refined carbohydrates and sugars galore to help them recover from the “damage” done by the high fat meal!
Blood samples were collected at 0 (baseline), 1, 3, and 6 h for the measurement of various substances, including the body fat hormones adiponectin and tumor necrosis factor-alpha levels.
The figure below shows the variation in adiponectin levels at several times after the meal. The black circles are for the high saturated fat group, and the white circles for the other group. Adiponectin levels do not really start at the same level for both groups, which makes the graph a bit unclear; to better interpret the graph it may be a good idea to simply ignore the first (white) circle at the zero mark on the vertical axis. Also, no hormone levels were negative, of course; the zero on the vertical axis represents a reference value.
As we can see from the figure above, adiponectin levels go up for both groups after the fatty meal, and end up higher than they started for both groups; more for the high saturated fat than for the low saturated fat group. They are at very similar levels at the 24 h mark, but the levels at 24 h for the high saturated fat group appear to be a lot higher than they were right after the fatty meal. (The start point for the high saturated fat group being the first black circle from the left on the graph.) None of the differences are reported as significant. This is not surprising, given the small sample.
The figure below shows the variation in tumor necrosis factor-alpha levels at several times after the meal. This is an even more interesting one, because it suggests a possible negative effect of the low fat meals.
In terms of tumor necrosis factor-alpha levels, the figure above suggests that both groups end up higher than they started, by about the same amount, which is not very good. (With tumor necrosis factor-alpha, unlike adiponectin, the less you have the better - so to speak, the hormone has important functions.) Again, none of the differences, with the exception of one, are reported as significant. The exception is the tumor necrosis factor-alpha level at 6 h for the low saturated fat group, which is significantly lower. But that difference disappears at the 10 h mark, never to be seen again.
Interestingly, note that tumor necrosis factor-alpha levels go up very clearly after the additional meals, which were low fat meals rich in refined carbohydrate and sugars. The variation in adiponectin is not as clearly associated with the additional meals. The points at which those meals were served are indicated by the arrows at the top of the graph; first arrow from left for lunch, second for a snack, and third arrow for dinner.
The conclusion by the authors of the study was that there is “… no evidence from this study of lean, healthy male subjects that the adipose hormone adiponectin is sensitive to acute intake of dietary lipid or to an increase in fatty acid saturation.” They do acknowledge the reduction in tumor necrosis factor-alpha up until the start of the low fat meals, and say that the “mechanism leading to the decrease in TNF-alpha on the high SFA:USFA treatment in our trial is unknown to us.”
My interpretation of this study is that, at least for young and lean men:
- There is some evidence that dietary saturated fat intake leads to increased levels of circulating adiponectin and decreased levels of tumor necrosis factor-alpha in the first few hours after a meal rich in saturated fat; with plenty of palmitic acid in it, by the way, of which animal fat is a great source. These are desirable and health-promoting hormonal responses.
- These is some evidence that meals high in refined carbohydrates and sugars increase levels of circulating tumor necrosis factor-alpha in the hours following the meals. Elevated levels of tumor necrosis factor-alpha are not good news; something that I guess is implied by the name of the hormone.
- There is some evidence that dietary saturated fat intake leads to an increase in adiponectin levels 24 h after a high fat meal, even when it is followed by low fat meals high in refined carbohydrates and sugars. This suggests a protective effect, which is in line with the hypothesis that adiponectin is not only a health marker by also a health-promoting hormone.
Due to the small sample used, none of the conclusions above is based on statistically significant results. More research is needed in the future, with larger samples. I am not sure it will happen though. This study’s findings were obviously accidental, and saturated fat phobia is still widespread.
Adiponectin is highly correlated with body weight, particularly weight associated with body fat mass. So, if you were able to achieve weight loss through a low carbohydrate diet involving a high consumption of saturated fat, there is absolutely no need to change that based on the results of this study.
Plus, saturated fat has the added benefit that it increases HDL cholesterol, the “good” cholesterol.
Reference:
Poppitt, S.D. et al. (2008). Postprandial response of adiponectin, interleukin-6, tumor necrosis factor-α, and C-reactive protein to a high-fat dietary load. Nutrition, 24(4), 322-329.
My final interpretation of the study results is a bit different though. It suggests that the results are actually the opposite of what the authors originally assumed.
The authors of the study (Poppitt et al., 2008; full reference at the end of this post) start by stating that since “… dietary fat is associated with increased lipid storage, weight gain, and obesity …” it is important to study the effect of dietary fat intake on the blood levels of certain substances that are associated with lipid disorders, weight gain and obesity.
In short, the authors start from the assumption that dietary fat is bad. By the way, this type of indictment of all fats is not very common these days. Usually saturated fat is the target.
Since dietary fat is assumed to be bad for us, that justifies the authors’ goal of studying the effect of dietary fat on certain hormones associated with bad health, including the body fat-secreted hormones adiponectin and tumor necrosis factor-alpha. Low levels of serum adiponectin, and elevated levels of tumor necrosis factor-alpha, are associated with various health complications.
In the study, a high-fat test meal with approximately 59 g of fat (71% of energy as fat) was given at breakfast on two occasions to 18 healthy and lean men. These men had, on average, 23 years of age, a 31-inch waist, and a body mass index of 22.9. In other words, they were young and fit.
Two fatty meal variations were used, one with a lot more saturated fat than the other. Their ratio of saturated:unsaturated fatty acids was 71:29 for the high saturated fat meal, and 55:45 for the other. The table below provides a more detailed picture of the fat composition of the meals. The authors refer to these meals as instances of “acute intake of dietary lipid”.
Lunch, snack and dinner meals were also served to the participants. Those meals were nearly fat-free, with 1 to 3 g of fat only; apparently to help the participants “recover” from the high fat meal. They included plenty of refined grains (e.g., pasta) and fruit juices. Way to go; give these folks refined carbohydrates and sugars galore to help them recover from the “damage” done by the high fat meal!
Blood samples were collected at 0 (baseline), 1, 3, and 6 h for the measurement of various substances, including the body fat hormones adiponectin and tumor necrosis factor-alpha levels.
The figure below shows the variation in adiponectin levels at several times after the meal. The black circles are for the high saturated fat group, and the white circles for the other group. Adiponectin levels do not really start at the same level for both groups, which makes the graph a bit unclear; to better interpret the graph it may be a good idea to simply ignore the first (white) circle at the zero mark on the vertical axis. Also, no hormone levels were negative, of course; the zero on the vertical axis represents a reference value.
As we can see from the figure above, adiponectin levels go up for both groups after the fatty meal, and end up higher than they started for both groups; more for the high saturated fat than for the low saturated fat group. They are at very similar levels at the 24 h mark, but the levels at 24 h for the high saturated fat group appear to be a lot higher than they were right after the fatty meal. (The start point for the high saturated fat group being the first black circle from the left on the graph.) None of the differences are reported as significant. This is not surprising, given the small sample.
The figure below shows the variation in tumor necrosis factor-alpha levels at several times after the meal. This is an even more interesting one, because it suggests a possible negative effect of the low fat meals.
In terms of tumor necrosis factor-alpha levels, the figure above suggests that both groups end up higher than they started, by about the same amount, which is not very good. (With tumor necrosis factor-alpha, unlike adiponectin, the less you have the better - so to speak, the hormone has important functions.) Again, none of the differences, with the exception of one, are reported as significant. The exception is the tumor necrosis factor-alpha level at 6 h for the low saturated fat group, which is significantly lower. But that difference disappears at the 10 h mark, never to be seen again.
Interestingly, note that tumor necrosis factor-alpha levels go up very clearly after the additional meals, which were low fat meals rich in refined carbohydrate and sugars. The variation in adiponectin is not as clearly associated with the additional meals. The points at which those meals were served are indicated by the arrows at the top of the graph; first arrow from left for lunch, second for a snack, and third arrow for dinner.
The conclusion by the authors of the study was that there is “… no evidence from this study of lean, healthy male subjects that the adipose hormone adiponectin is sensitive to acute intake of dietary lipid or to an increase in fatty acid saturation.” They do acknowledge the reduction in tumor necrosis factor-alpha up until the start of the low fat meals, and say that the “mechanism leading to the decrease in TNF-alpha on the high SFA:USFA treatment in our trial is unknown to us.”
My interpretation of this study is that, at least for young and lean men:
- There is some evidence that dietary saturated fat intake leads to increased levels of circulating adiponectin and decreased levels of tumor necrosis factor-alpha in the first few hours after a meal rich in saturated fat; with plenty of palmitic acid in it, by the way, of which animal fat is a great source. These are desirable and health-promoting hormonal responses.
- These is some evidence that meals high in refined carbohydrates and sugars increase levels of circulating tumor necrosis factor-alpha in the hours following the meals. Elevated levels of tumor necrosis factor-alpha are not good news; something that I guess is implied by the name of the hormone.
- There is some evidence that dietary saturated fat intake leads to an increase in adiponectin levels 24 h after a high fat meal, even when it is followed by low fat meals high in refined carbohydrates and sugars. This suggests a protective effect, which is in line with the hypothesis that adiponectin is not only a health marker by also a health-promoting hormone.
Due to the small sample used, none of the conclusions above is based on statistically significant results. More research is needed in the future, with larger samples. I am not sure it will happen though. This study’s findings were obviously accidental, and saturated fat phobia is still widespread.
Adiponectin is highly correlated with body weight, particularly weight associated with body fat mass. So, if you were able to achieve weight loss through a low carbohydrate diet involving a high consumption of saturated fat, there is absolutely no need to change that based on the results of this study.
Plus, saturated fat has the added benefit that it increases HDL cholesterol, the “good” cholesterol.
Reference:
Poppitt, S.D. et al. (2008). Postprandial response of adiponectin, interleukin-6, tumor necrosis factor-α, and C-reactive protein to a high-fat dietary load. Nutrition, 24(4), 322-329.
Monday, March 1, 2010
Adiponectin, inflammation, diabetes, and heart disease
Humans, like many animals, evolved to be episodic eaters and spend most of their time fasting. Body fat is the main store of energy in the human body. Excess dietary carbohydrates and fat are stored as body fat, in specialized cells known as adipocytes. Excess dietary protein is not normally stored as body fat.
Adipocytes can be seen as being part of a very important and distributed endocrine organ, being responsible for the release of many different hormones into the bloodstream. One of these hormones is adiponectin. Other important hormones secreted by body fat tissue are leptin and tumor necrosis factor-alpha.
Among hormones, adiponectin is particularly interesting because it is negatively correlated with body fat mass. That is, unlike other hormones such as leptin and tumor necrosis factor-alpha, a decrease in body fat mass (a well known health marker) is associated with an increase in adiponectin. This has led some researchers to speculate that adiponectin is a causative factor that promotes health, in addition to being a health marker.
Jung and colleagues (2008; full reference at the end of this post) studied 78 obese individuals (41 females) who participated in an exercise program during 12 weeks. The exercise program involved mostly low intensity aerobic activities, such as brisk walking. The individuals also took an appetite suppressant, with the goal of reducing their calorie intake by about 500 kcal per day.
The table below (click on it to enlarge) shows various measurements for the participants before and after the 12-week intervention.
Adipocytes can be seen as being part of a very important and distributed endocrine organ, being responsible for the release of many different hormones into the bloodstream. One of these hormones is adiponectin. Other important hormones secreted by body fat tissue are leptin and tumor necrosis factor-alpha.
Among hormones, adiponectin is particularly interesting because it is negatively correlated with body fat mass. That is, unlike other hormones such as leptin and tumor necrosis factor-alpha, a decrease in body fat mass (a well known health marker) is associated with an increase in adiponectin. This has led some researchers to speculate that adiponectin is a causative factor that promotes health, in addition to being a health marker.
Jung and colleagues (2008; full reference at the end of this post) studied 78 obese individuals (41 females) who participated in an exercise program during 12 weeks. The exercise program involved mostly low intensity aerobic activities, such as brisk walking. The individuals also took an appetite suppressant, with the goal of reducing their calorie intake by about 500 kcal per day.
The table below (click on it to enlarge) shows various measurements for the participants before and after the 12-week intervention.
From the table above we can say that there were significant reductions in weight, body mass index (BMI), waist and hip circumference, waist-to-hip ratio (WHR), total body fat, and total fasting cholesterol and triglycerides. However, the participants were still obese at the end of the intervention, with an average body fat percentage of 35.5.
The table below shows the concentrations of various hormones secreted by body fat tissue, as well as other types of tissue, before and after the 12-week intervention. These hormones are all believed to be health indicators and/or health causes.
The table below shows the concentrations of various hormones secreted by body fat tissue, as well as other types of tissue, before and after the 12-week intervention. These hormones are all believed to be health indicators and/or health causes.
We see from the table above that the hormonal changes were all significant (all at the P < .001 level except one, at the P < .05 level), and all indicative of health improvements. The serum concentrations of all hormones decreased, with two exceptions – adiponectin and interleukin-10, which increased. Interleukin-10 is an anti-inflammatory hormone produced by white blood cells. The most significant increase of the two was by far in adiponectin (P = .001, versus P = .041 for interleukin-10).
One of the most promising effects of adiponectin seems to be an increase in insulin sensitivity. This effect appears to be unrelated to any effects on insulin secretion. That is, adiponectin seems to act directly on various cells, including muscle cells, increasing their ability to clear glucose from the blood. This effect seems to be one of the underlying, and previously unknown, reasons why loss of body fat improves health in those who suffer from diabetes type 2.
Increased serum adiponectin has been found to be significantly associated with: decreased body fat and particularly visceral fat, decreased risk of developing diabetes type 2, decreased blood pressure, and decreased fasting triglycerides.
Adiponectin appears to also have anti-inflammatory and athero-protective properties.
On average, women have higher levels of serum adiponectin than men.
According to Giannessi and colleagues (2007) administration of adiponectin in mice has shown positive results. Since research on adiponectin is new, it will probably be some time until related drugs are developed. Giannessi and colleagues also note that fish oil and vanadium salts may increase the synthesis and release of adiponectin.
So far it seems that the most effective way of increasing adiponectin levels is weight loss, particularly through body fat loss. Even as new drugs are developed, this will likely remain the most natural and safe way of increasing adiponectin levels.
All of this helps in the identification of missing links between body fat loss and health improvement. It seems that losing body fat has an effect similar to that of supplementation; it increases the blood concentration of a health-promoting substance - adiponectin!
References:
Giannessi, D., Maltinti, M., & Del Ry, S. (2007). Adiponectin circulating levels: A new emerging biomarker of cardiovascular risk. Pharmacological Research, 56(6), 459-467.
Gil-Campos, M., Cañete, R., & Gil, A. (2004). Adiponectin, the missing link in insulin resistance and obesity. Clinical Nutrition, 23(5), 963-974.
Jung, S.H. et al. (2008). Effect of weight loss on some serum cytokines in human obesity: increase in IL-10 after weight loss. The Journal of Nutritional Biochemistry, 19(6), 371-375.
One of the most promising effects of adiponectin seems to be an increase in insulin sensitivity. This effect appears to be unrelated to any effects on insulin secretion. That is, adiponectin seems to act directly on various cells, including muscle cells, increasing their ability to clear glucose from the blood. This effect seems to be one of the underlying, and previously unknown, reasons why loss of body fat improves health in those who suffer from diabetes type 2.
Increased serum adiponectin has been found to be significantly associated with: decreased body fat and particularly visceral fat, decreased risk of developing diabetes type 2, decreased blood pressure, and decreased fasting triglycerides.
Adiponectin appears to also have anti-inflammatory and athero-protective properties.
On average, women have higher levels of serum adiponectin than men.
According to Giannessi and colleagues (2007) administration of adiponectin in mice has shown positive results. Since research on adiponectin is new, it will probably be some time until related drugs are developed. Giannessi and colleagues also note that fish oil and vanadium salts may increase the synthesis and release of adiponectin.
So far it seems that the most effective way of increasing adiponectin levels is weight loss, particularly through body fat loss. Even as new drugs are developed, this will likely remain the most natural and safe way of increasing adiponectin levels.
All of this helps in the identification of missing links between body fat loss and health improvement. It seems that losing body fat has an effect similar to that of supplementation; it increases the blood concentration of a health-promoting substance - adiponectin!
References:
Giannessi, D., Maltinti, M., & Del Ry, S. (2007). Adiponectin circulating levels: A new emerging biomarker of cardiovascular risk. Pharmacological Research, 56(6), 459-467.
Gil-Campos, M., Cañete, R., & Gil, A. (2004). Adiponectin, the missing link in insulin resistance and obesity. Clinical Nutrition, 23(5), 963-974.
Jung, S.H. et al. (2008). Effect of weight loss on some serum cytokines in human obesity: increase in IL-10 after weight loss. The Journal of Nutritional Biochemistry, 19(6), 371-375.
Multi-Sector Approaches to Pandemic Planning and Response:
A role for Arts and Culture?
The recent H5N1 and H1N1 viruses have raised our awareness that pandemics are not a myth of the distant past, but that they can quickly become concrete, actual threats to businesses, well-being and survival in multiple sectors across societies worldwide. What are the possible pandemic threats of the future and how can businesses, civil society and governments best prepare for these?
The recent H5N1 and H1N1 viruses have raised our awareness that pandemics are not a myth of the distant past, but that they can quickly become concrete, actual threats to businesses, well-being and survival in multiple sectors across societies worldwide. What are the possible pandemic threats of the future and how can businesses, civil society and governments best prepare for these?
I’m shortly going to be exploring ideas around this agenda with the Asia/Europe Foundation and I’d be interested to hear your opinions on how the arts and cultural sectors may play a part in this agenda. It might be about social marketing, or communicating risk; or it could be about how health services engage with communities and how these communities in turn, inform new ways of working.
This round table discussion is an opportunity for us to discuss what role the arts and culture can potentially play in this agenda.
If you would like to take part in this discussion please email me to register for a place ASAP.
Date: Tuesday 16th March
Time: 17:00 – 19:00
Venue: The Righton Building at MMU (see link below)
PLACES ARE STRICTLY LIMITED; RSVP as soon as possible to:
Subscribe to:
Posts (Atom)